Family Medicine Residency Program
Welcome!
Thank you for visiting our website and for your interest. As one of the most established Family Medicine Residency Programs in the country, West Suburban Medical Center offers residents the entire breadth of Family Medicine, with significant depth in each of many facets.
Our Faculty have been here for the long term, many with tenure in excess of 10-15 years. The Program devotes much attention to providing residents with a balance of supervision and autonomy, specific for the level of training. Achieving confidence, competence, and teaching and leadership skills by the time of graduation is of great importance.
West Suburban’s Family Medicine Residency Program continuously ranks among the highest in Illinois for the American Board of Family Medicine (ABFM) examination performance. We currently rank #2, in the state, for highest 5-Year Program Average, with a continuing 100% pass rate.
Only 9 miles west of downtown Chicago, there is much to explore outside the hospital; ensuring a healthy balance between professional and personal interests is viewed as critical to long-term success.
We welcome your questions and look forward to meeting you in person, through medical student clerkships or electives, or as an applicant to our program.
Questions about our Family Medicine Residency?
E-mail us: Program Administration: [email protected]
Melanie Jessen, DO
PROGRAM DIRECTOR
Program Strengths
West Suburban Medical Center offers all the advantages of a large medical center — in a community hospital setting. Our residents are exposed to challenging medical cases and collegial relationships with faculty. Our programs provide individually focused teaching from an enthusiastic faculty.
Other strengths include a thriving community hospital in an urban setting, an affiliation with Loyola Stritch School of Medicine, and Ann & Robert H. Lurie Children’s Hospital of Chicago. We provide a friendly work environment where there is no shortage of interesting medical, surgical, and obstetric cases, as well as a program that encourages active input from residents in decisions of direction and policy. As a graduate, you will leave the program with a well-grounded foundation in caring for patients and an appreciation of the community hospital atmosphere. This combination of community experience coupled with an academic perspective allows our residency programs to offer a wide variety of opportunities for residents to acquire competency in the skills necessary to provide patient care. The Family Medicine Residency Program is dually accredited by the Accreditation Council for Graduate Medical Education (ACGME) and the American Osteopathic Association (AOA).
The Family Medicine Residency Curriculum
Our Family Medicine Residency curriculum is designed to give you experience in a wide range of care. It will help prepare you to care for a diverse patient population throughout your health care career.
Program Locations
The West Suburban Family Medicine Residency Program accepts 10 first-year residents each year. The program assigns residents to one of four distinctive Family Medicine Center sites for their continuity clinic experiences. During the application process, students are oriented to the four centers: PCC Dr. Burdick Family Health Center, PCC Lake Street Family Health Center, PCC Austin Family Health Center, and PCC Salud Family Health Center. Once enrolled in the program, incoming residents indicate their site preference, and assignments are made by the Program Director.
PCC Community Wellness Center
PCC Community Wellness Center hosts the four clinical sites: one inside West Suburban Medical Center, one located in Oak Park, and two located in Chicago. In recognition of the need for community-based services for the medically indigent, PCC formed a community Board of Directors and was incorporated as a not-for-profit organization in June 1992. PCC was approved as a Federally Qualified Health Center (FQHC) look-alike in 1994 and an FQHC in 2002. The mission of PCC is to improve health outcomes for the medically underserved community through the provision of high quality, affordable, and accessible primary health care and support services. PCC accepts all patients regardless of their ability to pay.
PCC Dr. Burdick Family Health Center – West Suburban Medical Center Site
Initially known as West Suburban’s Family Medicine Center, this site was accredited in 1972 and is assigned four new residents per year for a total of twelve residents at the site. This is the residency’s first training site and also serves as the location of the residency program’s administrative offices. The characteristics of the patients of this site reflect the heterogeneous nature of the population of the surrounding communities it serves. There is a full demographic range in education and income. Most adult patients are currently employed, and many patient visits are by members of managed health care plans. There is a significant demographic mixture of patients in culture, age, and gender. In the majority of cases, more than one family member receives care at this Center.
On September 17, 2009, nearly 100 physicians and family members attended the dedication of West Suburban Medical Center’s Family Medicine Center in honor of Dr. A.L. Burdick, founder of the Family Medicine Residency Program. Dr. Burdick was a visionary, a national leader, and one of the founding fathers of the Family Medicine movement in the United States. Dozens of doctors, now practicing family medicine physicians, traveled from as far as Maine to honor their mentor and pay tribute to Dr. Burdick’s extraordinary career. The site was acquired by PCC on September 1, 2022.
PCC Lake Street Family Health Center – Oak Park Site
The PCC Lake Street Family Health Center was accredited as a Family Medicine Center in 1994. The Center was founded in April 1980 and is assigned two new residents per year for a total of six residents at the site. It is located on the border of Chicago and Oak Park, Illinois. PCC’s primary service area is the Chicago community of Austin, and also a significant portion of the communities of West and East Garfield Park, Humboldt Park and North Lawndale.
PCC Salud Family Health Center – Chicago Site
The PCC Salud Family Health Center was accredited as a Family Medicine Center in 1997 and is assigned two new residents per year for a total of six residents at the site. This center serves patients primarily from Chicago’s northwest side communities of Belmont/Cragin, Hermosa, Humboldt Park, West Town and Austin. The patient population is largely working class. The PCC Salud Family Health Center is one of the few medical facilities in the area with Spanish-speaking health care providers, and thus enjoys a growing Hispanic patient base. Residents selecting Salud as a Family Medicine Center are an integral part of its development as a residency-training site. Spanish-speaking ability is preferred, but not required.
PCC Austin Family Health Center – Chicago Site
The PCC Austin Family Health Center serves the Austin community—a predominantly African American and impoverished community of Chicago’s west side. On January 25, 2010, the facility moved to a new and larger location. The new facility provides double the exam room space than the original location, provides expanded behavioral health and oral health services, and houses a 340B Pharmacy Program. In May 2010, the Austin Family Health Center was approved as our fourth continuity clinic site by the Accreditation Council for Graduate Medical Education. Since July 2010, two new residents are assigned at this site per year for a total of six residents at the site.
Videos
Why West Sub?
A 2017 Graduate’s Advice to Students Seeking Residency Programs in 2020-2021
Patricia Martin, DO
Assistant Program Director
RWJUH Somerset Family Medicine Residency
Somerville, NJ
Reflections From Our 2019 Graduates
IAFP 2020 Awards Ceremony
What a Year for West Suburban Alumni!
Family Physician of the Year
Alyssa Jeanne Vest Hart, DO, FAAFP
Class of 2009
Family Medicine Teacher of the Year
Carl Earl Lambert, Jr., MD, FAAFP
Class of 2014
Resident Teacher of the Year
Joanna Curran, MD
Class of 2020
IAFP President’s Award
Raj C. Shah, MD
Class of 2000
Congratulations to our West Suburban Medical Center Family Medicine Residency Program alumni!
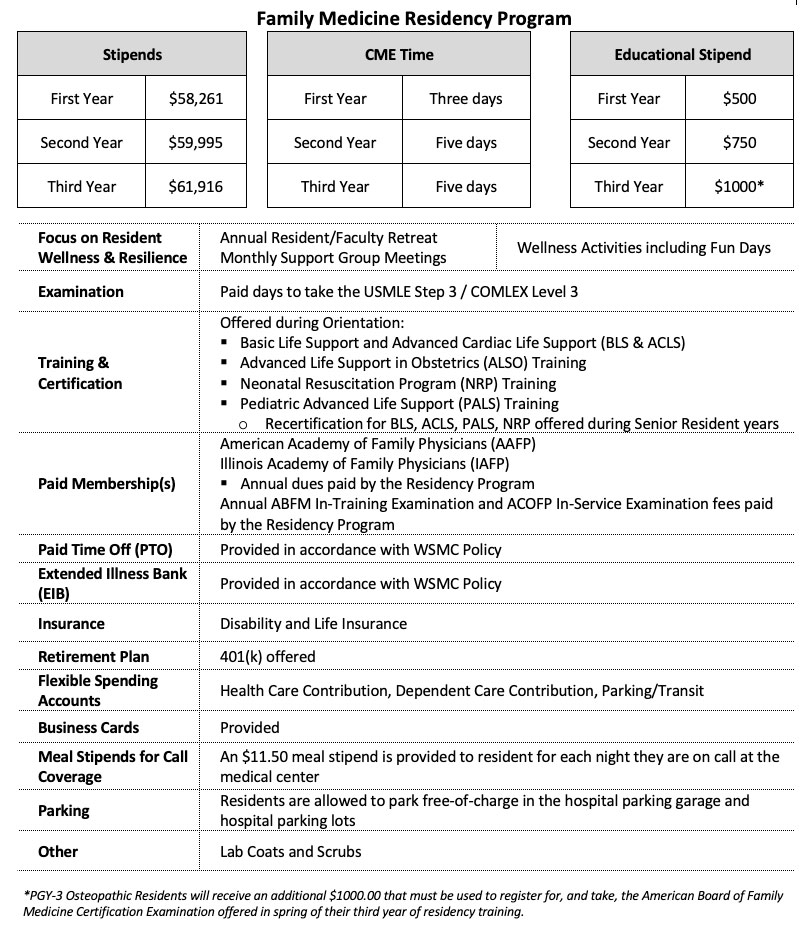
Benefits & Stipends
Apply to Our Program
All three years of the West Suburban Family Medicine Residency Program are accredited by the ACGME to bring only the best students to our program.
We accept applications only through the Electronic Residency Application Service (ERAS). Your medical school dean’s office or the Educational Commission for Foreign Medical Graduates (ECFMG) will provide information about how you can access this process.
After we receive your complete ERAS application, our Recruitment Committee will review your file. If your application meets our selection criteria, the Program Assistant will invite you, via e-mail, to schedule an interview. Interview appointments are scheduled November through mid-January. We look forward to hearing from you!
Additional Information for the Applicant:
- 10 first-year resident positions are offered each academic year.
- Our program participates in the National Resident Matching Program (NRMP).
- Applications are accepted through the Electronic Residency Applicant Service (ERAS) only.
- NRMP Match Code 1173120C0
- All candidates must be United States citizens or Permanent Residents. We do not sponsor or accept any visas, even visas sponsored by the Educational Commission for Foreign Medical Graduates (ECFMG) Exchange Visa Sponsorship Program (EVSP).
- All applicants must possess excellent written and oral communication skills.
- Graduation from medical school within the past three years
- Applicants with two or more attempts on any portion of the USMLE or COMLEX exam are less likely to be considered for an interview. Osteopathic applicants may submit USMLE or COMLEX scores.
- Dean’s Letter (also known as the Medical Student Performance Evaluation) is required.
- Three (3) current letters of recommendation (written within the past 12 months) are required. At least one letter should be from a Family Physician.
- Medical School Transcript and Personal Statement are required.
- All documents must have certified translations if not in English.
- Applicants selected to interview are notified by e-mail.
- Interviews are conducted November through January
- Final application deadline (including receipt of all required documents) is December 1st.
- The screening process does not consider gender, sexual orientation, age, race, religion, ethnic origin, economic status, veteran status, or place of residence.
- All prospective employees must pass a criminal background check and drug screen.
Additional Information for International Medical Graduates:
- Applicants must have one year (1 year) of current clinical experience in the United States: completion of clinical rotations in the United States within the past two years, precepted by a licensed allopathic or osteopathic physician, may fulfill this requirement. Research does not substitute for clinical experience.
- Applicants must have received, or be eligible for, a currently valid ECFMG Certificate.
Questions about our Family Medicine Residency? E-mail us: Program Administration.

